AbstractSyncope is defined as a transient loss of consciousness due to cerebral hypoperfusion with spontaneous return to baseline function without intervention. It is a common chief complaint of patients presenting to the emergency department. The differential diagnosis for syncope is broad and the management varies significantly depending on the underlying etiology. In the emergency department, determining the cause of a syncopal episode can be difficult. However, a thorough history and certain physical exam findings can assist in evaluating for life-threatening diagnoses. Risk-stratifying patients into low, moderate and high-risk groups can assist in medical decision making and help determine the patient’s disposition. Advancements in ambulatory monitoring have made it possible to obtain prolonged cardiac evaluations of patients in the outpatient setting. This review will focus on the diagnosis and management of the various types of syncope.
INTRODUCTIONSyncope is a common chief complaint encountered in the emergency department (ED). The causes of syncope range from benign to life threatening. Being able to rule out life threatening causes is one of the main goals of the emergency physician. A fundamental understanding of the various types of syncope along with a thorough history and physical exam help identify the etiology of a patient’s syncopal episode. This review will focus on defining the types of syncope, identifying key components of the history and physical exam, and utilizing risk-stratification to safely disposition these patients.
EPIDEMIOLOGYSyncope is a common yet vague complaint of patients presenting to the ED. Approximately 1% to 2% of all ED visits occur due to a chief complaint of syncope, which amounts to around 1 million patient visits per year [1]. Half of these patients are admitted to the hospital for further testing; within the admitted subset half will be discharged with no clear diagnosis [2]. The US healthcare system spends 2.5 billion dollars per year on hospitalizations alone for syncope related admissions [3]. Many patients undergo extensive testing that has low diagnostic yield and often fails to diagnose the underlying etiology [4]. This leads to the question of whether such aggressive, costly and time-consuming investigations are justifiable for all patients presenting with syncope and how to risk-stratify patients so those at higher risk for adverse outcomes are appropriately identified and receive the proper work-up.
DEFINITIONSyncope is a symptom and not a diagnosis. Properly defined, syncope is a transient loss of consciousness with return to baseline neurological function without medical intervention. The pathophysiology of a syncopal episode is the same regardless of the cause. Syncope occurs due to a period of global hypoperfusion of the cerebral cortex or focal hypoperfusion of the reticular activating system that results in a loss of consciousness. Patients with loss of consciousness that have a persistent alteration in mental status, new neurological complaints or loss of consciousness that is related to alcohol or illicit drugs are not classified as true syncope.
Syncope vs. near syncopeNear syncope is a spectrum of syncope and should be approached similarly. The key difference is that in near syncope the hypoperfusion of the brain does not result in loss of consciousness. The mechanism and causes of near syncope are identical to syncope [5]. In general, patients with near syncope tend to be younger and have fewer comorbidities. Although patients with near syncope have about half as many serious outcomes—including arrhythmias and death—the occurrence of these outcomes is still significant [6]. Near syncope has a less dramatic presentation and is often under appreciated leading to fewer investigations and relatively more missed outcomes compared to patients who present with syncope [5-7].
Causes of syncopeThe differential diagnoses for syncope is broad and management is focused on the underlying cause when identifiable. During the ED visit only about half of patients will have a clear etiology determined. A thorough history and physical exam leads to improved diagnoses [8]. Risk stratifying the remaining patients into high and low risk groups can help with disposition. Being able to differentiate between the various types of syncope can impact the management of care and the ultimate disposition of patients that present to the ED.
The primary objective is to determine whether a patient has a life-threatening cause of syncope and to appropriately manage those conditions. Conditions such as acute hemorrhage, pulmonary embolism, and subarachnoid hemorrhage are important and clinically apparent causes of syncope upon presentation. Cardiac causes, especially occult arrhythmias, can be life threatening and not as obvious on presentation. This review will focus on the diagnosis and management of the different types of syncope, including cardiac syncope caused by arrhythmias.
CLASSIFICATIONSyncope can be broken down into 5 main categories: neurocardiogenic, orthostatic, neurological, cardiac and unknown causes (Table 1). Vasovagal syncope, also referred to as neurocardiogenic syncope, is the most common cause of syncope [9]. This type of syncopal episode occurs due to inappropriate vasodilation of the vascular system or due to bradycardia that leads to cerebral hypoperfusion and loss of consciousness. Most patients will describe prodromal symptoms of nausea, diaphoresis, or a lightheaded sensation prior to losing consciousness. Patients with vasovagal syncope have no increase in morbidity or mortality after their syncopal episode [10]. Vasovagal syncope can be precipitated by events that increase vagal tone such as micturition or defection. Situational syncope is an example of vasovagal syncope that occurs after events like phlebotomy or prolonged standing. Another example is irritation of the carotid sinus from activities, such as lateral head movement or shaving, that lead to stimulation of the vagal nerve which ensheaths the carotid arteries.
Orthostatic syncope is defined as postural hypotension that results in a syncopal episode. Orthostatic vitals are defined as a reduction in systolic blood pressure by 20 mmHg or a reflex tachycardia of more than 20 beats per minute. Causes include dysfunction of the autonomic nervous system and intravascular volume loss due to decreased intake or excessive output from the gastrointestinal tract. Orthostatic syncope is a diagnosis of exclusion that is reserved for low risk patients. Orthostatic vitals should be interpreted with caution as cardiogenic syncope can also present with orthostatic vitals signs. Orthostatic vitals are not sensitive or specific in diagnosing syncope or assessing a patient’s volume status since many patients who meet the definition of orthostasis do not have syncopal episodes [11,12]. Patients more likely to have orthostatic syncope include the elderly, pregnant women, and patients taking vasodilatory medications. Medications can cause syncope due to cardiotoxicity or from side effects of over-medication, such as excessive diuretics or an inappropriately high dose of antihypertensives.
Neurologic syncope is the least common cause of syncope [9]. Causes include seizures, transient ischemic events, subclavian steal syndrome and complex migraine headache. A failure to return to baseline does not qualify as syncope and should be worked up for alternative causes. In addition, patients with new neurological deficits do not fall under this category.
Cardiac syncope is the most common life-threatening cause of syncope. Potential causes include arrhythmias, valvular heart disease, myocardial infarction, cardiac tamponade, or pacemaker malfunction (Table 2). Patients with arrhythmias may have tachy- or brady-arrhythmias. Tachyarrhythmias that cause syncope and lead to sudden cardiac death include ventricular tachycardia, ventricular fibrillation, and Wolff-Parkinson-White with supraventricular tachycardia. Atrial fibrillation and atrial flutter can also cause syncope but will rarely lead to sudden death. Bradycardias occur due to conduction delays resulting from sinus or atrioventricular node dysfunction which causes impaired transmission of the electrical impulse and can result in heart blocks. Concerning bradycardias such as Mobitz II or type 3 atrioventricular blocks need urgent evaluation and possible pacemaker placement as they can lead to sudden cardiac death. Obstructive lesions such as severe aortic stenosis or mitral stenosis can cause exertional syncope. The underlying mechanism isn’t definitively known but it is believed that the stenosis results in a fixed cardiac output that cannot be increased during periods of exertion. During exertion, peripheral vasodilation occurs to increase blood flow to the skeletal muscles. When there isn’t an increase in cardiac output due to the fixed valvular stenosis, the peripheral vasodilation causes a transient hypotension, which results in cerebral hypoperfusion and syncope. Patients that present with cardiac syncope have a 30% increased risk of sudden death within one year [9,13]. Patients with a history of heart failure have an even higher mortality [14].
Patients with an unknown cause of syncope have 30% higher mortality than patients who have not had a syncopal episode [10]. In this subgroup, determining whether the patient has an underlying heart condition can assist in identifying high-risk patients. In addition, patients should be evaluated for other life-threatening diagnoses that can present with syncope such as pulmonary embolism, internal hemorrhage, or cerebrovascular accident.
EMERGENCY DEPARTMENT MANAGEMENTIn the ED setting, patients that present with syncope can be risk stratified to determine who needs further investigation. Patients with apparent neurologic or cardiac causes should be admitted. Patients with vagal and orthostatic syncope can be safely discharged once medically optimized. In the remaining patients, the question to consider is who is at risk for a lethal arrhythmia and whether this is something that can be accurately predicted. The answer to this question helps guide which patients need further investigation.
HISTORY AND PHYSICAL EXAMA thorough history can provide valuable information in determining the etiology of a syncopal episode. An important historical clue is the presence of associated symptoms prior to the episode. A patient with preceding angina may have an acute coronary syndrome while a patient with dyspnea should be evaluated for pulmonary embolism or cardiac tamponade. A patient with a preceding headache may be presenting with a subarachnoid hemorrhage.
Patients with prodromal symptoms such as nausea, diaphoresis, or pallor are more likely to have neurocardiogenic syncope. In addition, activities prior to the start of the prodromal symptoms such as micturition or coughing should be elicited as potential triggers. Identifying these patients is helpful as they have a more benign course and can be discharged without further testing and with no increase in morbidity and mortality.
Conversely, patients with sudden loss of consciousness without prodromal symptoms are more likely to have had an arrhythmia [6]. Syncope with exertion can be a sign of an underlying cardiac abnormality such as a valvular defect, an aortic outflow obstruction, or a channelopathy that predisposes to arrhythmias. Syncope with positional change can occur due to orthostasis or neurocardiogenic causes such as prolonged standing, hypovolemia or autonomic dysregulation [15].
Historical factors that are strongly associated with cardiac syncope include a strong family history of sudden death or early myocardial infarction before 50 years of age, a history of heart disease (heart failure, myocardial infarction, valvular disease, and arrhythmias) and presenting symptoms suggestive of heart disease (chest pain, palpitations, and shortness of breath) [16-18]. In addition, the patient’s medications should be carefully reviewed as this can be a source of syncope for a significant number of patients.
Physical exam should focus on the patient’s vital signs and thorough neurologic and cardiac examinations. Vital signs during the syncopal episode itself are usually abnormal with transient hypotension or bradycardia. By the time of evaluation, the vitals have usually normalized. Persistently abnormal vitals may indicate an underlying cause; for example, hypoxia and tachypnea may indicate heart failure or pulmonary embolism. Cardiac exam may reveal a murmur such as the mid-systolic click of aortic stenosis or an abnormal rhythm such as atrial fibrillation. Neurologic exam should be normal in a patient with a true syncopal episode, and any focal abnormalities should be further investigated for a cerebrovascular accident. Additional findings on physical exam that can lead to the underlying diagnoses include carotid bruits, a positive hemoccult test suggesting gastrointestinal bleeding, and intraoral lacerations suggestive of seizure.
INVESTIGATIONSThe presentation and clinical scenario helps to guide the extent of the ED investigation. An electrocardiogram (ECG) should be done on most patients since it is both cost-effective, non-invasive and has been shown to help risk-stratify patients [19]. Hematologic studies or advanced imaging, including computed tomography scans, can be ordered based on the history and exam. Women of childbearing age should be evaluated for pregnancy. Electrolytes and hematocrit can be assessed in a patient with a history of diarrhea and vomiting or gastrointestinal hemorrhage respectively. A patient that is low risk usually gets little to no advanced investigations when admitted. Higher risk patients may need prolonged cardiac monitoring to evaluate for potential arrhythmias and an echocardiogram to identify structural heart disease [20]. Echocardiography is likely the most useful test to help risk stratify patients as it can identify those that have structural heart disease including valvular abnormalities, wall motion abnormalities and pericardial effusions [21].
Electrocardiogram abnormalitiesCertain ECG changes are more valuable than others in predicting patients at higher risk. The ECG may indicate changes consistent with ischemia or arrhythmia. Three percent of syncope patients are found to have a myocardial infarction and usually present with atypical symptoms and non-ST elevations on their initial ECGs [19]. A patient with a non-sinus rhythm or any abnormal conduction of the left bundle—including left bundle branch block, left anterior fascicular block, left posterior fascicular block, or QRS interval widening—is at greater risk for significant cardiac outcomes [19]. The European Society of Cardiology identifies potential ECG abnormalities that can lead to cardiac syncope, such as prolonged intervals (QRS interval, QTc), severe bradycardia, and evidence of pre-excitation (Wolff-Parkinson-White) [22]. Other ECG findings include low voltage or electrical alternans as seen in pericardial effusion and abnormal conduction syndromes due to channelopathies.
Patients with certain genetic diseases that causes abnormal function of the cardiac ion channels such as Brugada, prolonged QT, short QT or catecholaminergic polymorphic ventricular tachycardia are more susceptible to sudden cardiac death [23]. During asymptomatic periods, patients with QT changes or catecholaminergic polymorphic ventricular tachycardia will have normal ECGs and no underlying structural heart disease identified on echocardiography, which can make diagnosis difficult. The abnormal channelopathy can sometimes be uncovered during stress testing. Genetic testing in patients with unexplained syncope or a family history of sudden cardiac death has recently been utilized to help identify patients with mutations that predispose them to fatal arrhythmias.
RISK STRATIFICATIONRegardless of etiology, patients with syncope have a higher mortality rate than those without [10]. In addition, a patient that presents with syncope has an increased risk of death and cardiovascular morbidity at one year [24,25]. A syncopal episode itself does not have a direct causality with increased mortality. Patients with underlying structural heart disease, ECG abnormalities, advanced age, and lack of prodromal symptoms are at increased risk for morbidity and mortality [18,24]. On the other hand, patients less than 45 years of age with no cardiac history are at lower risk [24]. Elderly patients are more likely to be on multiple medications and have orthostasis or autonomic dysfunction. Studies differ on the optimal age at which patients are at increased risk for adverse outcomes. In general, a patients’ age should be used as a guide with increasing risk of morbidity and mortality as age increase. In addition, the age should be considered within the context of other underlying medical problems that puts the patient at increased risk.
San Francisco Syncope RuleThe San Francisco Syncope Rule is a rule that can help risk stratify patients with syncope and identify patients who may be at a higher risk of adverse outcomes (Table 3) [26]. The rule was developed prospectively and has been validated with 1,400 ED patients. Fifty clinical variables were evaluated of which 5 were determined to be statistically significant in predicting patients who had a higher chance of adverse outcomes and warranted inpatient admission. The five variables include the following: history of congestive heart failure, an abnormal ECG or rhythm strip, shortness of breath, hematocrit <30, and systolic blood pressure <90 mmHg. Patients that meet any of these 5 criteria are predicted to be at higher risk for adverse outcomes, including mortality, at 7 days. Adverse outcomes include death, myocardial infarction, arrhythmia, pulmonary embolism, stroke, subarachnoid hemorrhage, or significant hemorrhage. The rule has a 74% to 98% specificity and a 56% sensitivity [26]. Subsequent studies that attempted to validate the SFSR resulted in lower sensitivities [27,28]. However, these studies tended to have patients with more neurological outcomes, did not use the same definition of syncope for study enrollment, used varying criteria for abnormal ECGs or arrhythmia, and did not consider rhythm abnormalities that occurred after the initial ECG—such as in the ED while being monitoring or on subsequent ECG’s.
DISPOSITIONPatients with identified neurologic or cardiac causes of syncope should usually be admitted for further investigation or treatment. High-risk patients should be admitted to an inpatient or observation unit for monitoring, or alternatively have close outpatient follow-up with ambulatory cardiac monitoring (Fig. 1).
Value of hospitalizationIt is difficult to create a generalized approach to patients that present with syncope. Hospitals in different regions, both nationally and internationally, operate with varying inpatient and outpatient resources as well as medical-legal climates. Within the United States, syncope admissions vary widely; academic centers have admission rates ranging from 55% to 85% while health maintenance organization’s with close outpatient follow-up admit close to 35% [2]. There is much international variability amongst admission rates with countries like Australia admitting <30% and Canada admitting <20% of their syncope patients. Regardless of the differing admission rates, these patients have no real differences in outcome [2,3] and it is unclear if hospitalization has any impact in reducing morbidity or mortality in patients with an unclear etiology of their syncope [20,30]. The need for admission should be based on the level of concern given each individual patient’s history and exam.
The best way to determine the need for hospitalization is to attempt to risk-stratify patients into low, moderate, and high-risk groups (Fig. 1). As described earlier, low risk patients include those that are younger and have prodromal symptoms prior to the episode, not including chest pain or dyspnea. These patients do not require any hospitalization and don’t require any specific follow-up or outpatient work-up unless symptoms are recurrent. Intermediate risk patients can be categorized based on the clinical suspicion for arrhythmia and the frequency of symptoms. High-risk patients include those with a history of heart disease (both structural and/or acute coronary syndrome), those with concerning ECG changes, advanced age, or prodromal symptoms such as syncope with exertion and new onset angina or dyspnea. Intermediate risk patients that are hemodynamically stable may benefit from an ED observational unit; leading to decreased hospital costs and total length of stay without adversely impacting clinical outcomes [31,32]. High-risk patients can be monitored in an observational unit or directly admitted to the hospital for further work-up and interventions. High and intermediate risk patients that are found to have concerning arrhythmias during the observation period should be admitted for further testing or intervention. In one study following 95 syncope patients, the majority of abnormalities found on 24-hour Holter recordings included bradycardia <30 beats per minute, sinus pauses >2 seconds, Mobitz II conduction block, complete heart block, ventricular tachycardia, and premature ventricular contractions [33]. These findings suggest an arrythmogenic cause of syncope and warrant inpatient admission and further workup.
Ambulatory monitoring: who to monitorLow risk patients that have a negative work up in the ED do not need ambulatory monitoring; however, it may provide reassurance especially for patients with recurrent syncopal episodes or symptoms of palpitations and lightheadedness. These patients can be discharged with expedited follow-up and ambulatory monitoring as warranted. Patients that are intermediate risk may also require ambulatory monitoring but this can be guided by the clinical suspicion for an arrhythmia and the inpatient or outpatient resources available. Patients that are high risk warrant in-patient admission and may also benefit from prolonged ambulatory monitoring if 24 to 48 hours of inpatient telemetry is normal.
There are many different types of devices available to monitor patients for arrhythmias (Table 4). Advancements in cardiac monitoring have made it possible to perform extended monitoring of patients in ambulatory settings than was previously attained during a hospital stay. Newer devices are more compact and comfortable, increasing patient compliance and providing more data [34]. Devices include event monitors, loop recorders, mobile cardiac telemetry systems, and long-term continuous rhythm recorders (such as the Zio Patch). These ambulatory monitoring devices make it easier to obtain prolonged telemetry readings and assess for arrhythmias. These devices may help decrease the number of inpatient admissions and increase the total length of time that a patient’s cardiac rhythm is observed—leading to a higher probability of diagnosing an arrhythmia.
Future researchThe large amount of research done on syncope has yielded some common risk factors that place patients at risk for adverse outcomes after a syncopal episode. Notably, advanced age, ECG changes, and underlying heart disease continue to be the best determinants for risk-stratifying patients. Cardiac syncope is the most concerning etiology as it can lead to sudden death following a fatal arrhythmia. Future research should be aimed at attempting to identify patients with arrhythmias. We now have devices that can be used to monitor patients conveniently for prolonged periods. Having a clear method to determine arrhythmia outcomes will be important in all future research.
CONCLUSIONAs discussed above, the patient with syncope can be appropriately managed and dispositioned using proper risk stratification guidelines. These guidelines assist in optimizing patient care while also keeping health care costs down. The most important determination is classifying patients into the appropriate risk group. Advances in science and technology have enabled genetic testing and prolonged cardiac monitoring devices which help to identify patients with life threatening causes with less resources and more efficiency than previously.
REFERENCES1. Sun BC, Emond JA, Camargo CA Jr. Direct medical costs of syncope-related hospitalizations in the United States. Am J Cardiol 2005; 95:668-71.
2. Quinn JV. Yield of diagnostic tests in evaluating syncopal episodes in older patient: invited commentary. Arch Intern Med 2009; 169:1305-6.
3. Sun BC, Emond JA, Camargo CA Jr. Characteristics and admission patterns of patients presenting with syncope to U.S. emergency departments, 1992-2000. Acad Emerg Med 2004; 11:1029-34.
4. Chiu DT, Shapiro NI, Sun BC, Mottley JL, Grossman SA. Are echocardiography, telemetry, ambulatory electrocardiography monitoring, and cardiac enzymes in emergency department patients presenting with syncope useful tests? A preliminary investigation. J Emerg Med 2014; 47:113-8.
5. Quinn JV. Syncope and presyncope: same mechanism, causes, and concern. Ann Emerg Med 2015; 65:277-8.
6. Krahn AD, Klein GJ, Yee R, et al. Predictive value of presyncope in patients monitored for assessment of syncope. Am Heart J 2001; 141:817-21.
7. Thiruganasambandamoorthy V, Stiell IG, Wells GA, Vaidyanathan A, Mukarram M, Taljaard M. Outcomes in presyncope patients: a prospective cohort study. Ann Emerg Med 2015; 65:268-76; e6.
9. Brignole M, Menozzi C, Bartoletti A, et al. A new management of syncope: prospective systematic guideline-based evaluation of patients referred urgently to general hospitals. Eur Heart J 2006; 27:76-82.
10. Soteriades ES, Evans JC, Larson MG, et al. Incidence and prognosis of syncope. N Engl J Med 2002; 347:878-85.
11. Koziol-McLain J, Lowenstein SR, Fuller B. Orthostatic vital signs in emergency department patients. Ann Emerg Med 1991; 20:606-10.
12. Sarasin FP, Louis-Simonet M, Carballo D, Slama S, Junod AF, Unger PF. Prevalence of orthostatic hypotension among patients presenting with syncope in the ED. Am J Emerg Med 2002; 20:497-501.
13. Linzer M, Yang EH, Estes NA 3rd, Wang P, Vorperian VR, Kapoor WN. Diagnosing syncope. Part 1: value of history, physical examination, and electrocardiography. Clinical Efficacy Assessment Project of the American College of Physicians. Ann Intern Med 1997; 126:989-96.
14. Middlekauff HR, Stevenson WG, Stevenson LW, Saxon LA. Syncope in advanced heart failure: high risk of sudden death regardless of origin of syncope. J Am Coll Cardiol 1993; 21:110-6.
15. Calkins H, Shyr Y, Frumin H, Schork A, Morady F. The value of the clinical history in the differentiation of syncope due to ventricular tachycardia, atrioventricular block, and neurocardiogenic syncope. Am J Med 1995; 98:365-73.
16. Martin TP, Hanusa BH, Kapoor WN. Risk stratification of patients with syncope. Ann Emerg Med 1997; 29:459-66.
17. Oh JH, Hanusa BH, Kapoor WN. Do symptoms predict cardiac arrhythmias and mortality in patients with syncope? Arch Intern Med 1999; 159:375-80.
18. Colivicchi F, Ammirati F, Melina D, et al. Development and prospective validation of a risk stratification system for patients with syncope in the emergency department: the OESIL risk score. Eur Heart J 2003; 24:811-9.
19. Quinn J, McDermott D. Electrocardiogram findings in emergency department patients with syncope. Acad Emerg Med 2011; 18:714-8.
20. Mendu ML, McAvay G, Lampert R, Stoehr J, Tinetti ME. Yield of diagnostic tests in evaluating syncopal episodes in older patients. Arch Intern Med 2009; 169:1299-305.
21. Sarasin FP, Junod AF, Carballo D, Slama S, Unger PF, Louis-Simonet M. Role of echocardiography in the evaluation of syncope: a prospective study. Heart 2002; 88:363-7.
22. Brignole M, Alboni P, Benditt D, et al. Guidelines on management (diagnosis and treatment) of syncope. Eur Heart J 2001; 22:1256-306.
23. Herman A, Bennett MT, Chakrabarti S, Krahn AD. Life threatening causes of syncope: channelopathies and cardiomyopathies. Auton Neurosci 2014; 184:53-9.
24. Kapoor WN, Karpf M, Wieand S, Peterson JR, Levey GS. A prospective evaluation and follow-up of patients with syncope. N Engl J Med 1983; 309:197-204.
25. Linzer M, Yang EH, Estes NA 3rd, Wang P, Vorperian VR, Kapoor WN. Diagnosing syncope. Part 2: unexplained syncope. Clinical Efficacy Assessment Project of the American College of Physicians. Ann Intern Med 1997; 127:76-86.
26. Quinn JV, Stiell IG, McDermott DA, Sellers KL, Kohn MA, Wells GA. Derivation of the San Francisco Syncope Rule to predict patients with short-term serious outcomes. Ann Emerg Med 2004; 43:224-32.
27. Thiruganasambandamoorthy V, Hess EP, Alreesi A, Perry JJ, Wells GA, Stiell IG. External validation of the San Francisco Syncope Rule in the Canadian setting. Ann Emerg Med 2010; 55:464-72.
28. Birnbaum A, Esses D, Bijur P, Wollowitz A, Gallagher EJ. Failure to validate the San Francisco Syncope Rule in an independent emergency department population. Ann Emerg Med 2008; 52:151-9.
29. Sarasin FP, Hanusa BH, Perneger T, Louis-Simonet M, Rajeswaran A, Kapoor WN. A risk score to predict arrhythmias in patients with unexplained syncope. Acad Emerg Med 2003; 10:1312-7.
30. Costantino G, Dipaola F, Solbiati M, Bulgheroni M, Barbic F, Furlan R. Is hospital admission valuable in managing syncope? Results from the STePS study. Cardiol J 2014; 21:606-10.
31. Sun BC, McCreath H, Liang LJ, et al. Randomized clinical trial of an emergency department observation syncope protocol versus routine inpatient admission. Ann Emerg Med 2014; 64:167-75.
32. Shen WK, Decker WW, Smars PA, et al. Syncope Evaluation in the Emergency Department Study (SEEDS): a multidisciplinary approach to syncope management. Circulation 2004; 110:3636-45.
Fig. 1.Algorithm for the approach to patients presenting to the emergency department (ED) with syncope. a)High risk criteria: abnormal electrocardiogram, including non-sinus rhythm while in ED; history of or findings of cardiovascular disease, especially congestive heart failure or structural heart disease; absence of prodromal/vagal symptoms; persistent low blood pressure (systolic blood pressure <90 mmHg); family history of sudden cardiac death (especially in younger patients); advanced age. 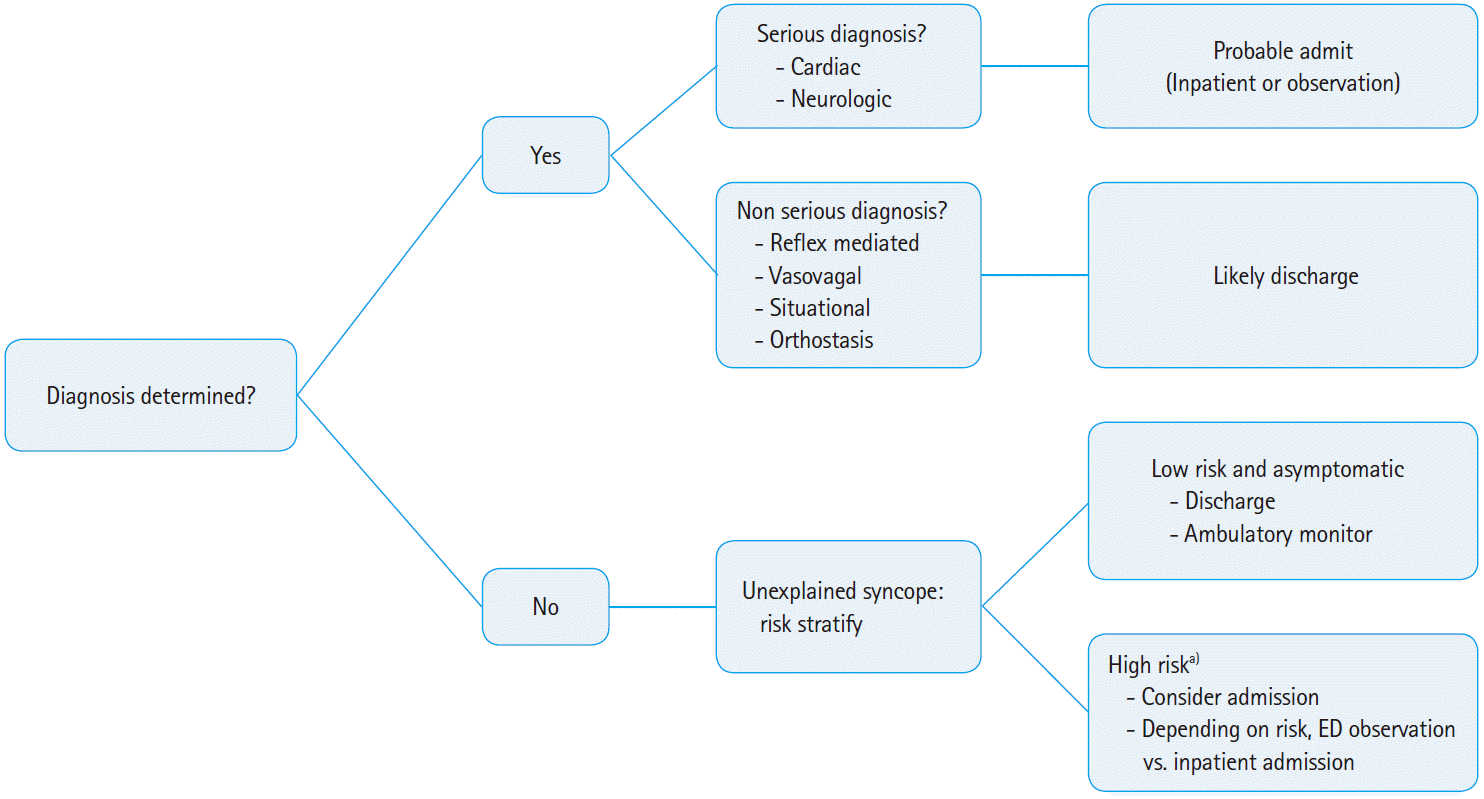
Table 1.Etiology of syncope: five classes of syncope defined by their associated causes or triggers Table 2.Cardiac etiologies of syncope: example of the most common causes of syncope based on underlying cardiac etiology Table 3.San Francisco Syncope Rule Risk stratifies patients into high and low risk. Patients that meet the above five are at higher risk for adverse outcomes within 7 days and increased mortality. Abnormal electrocardiogram (ECG) changes include non-sinus rhythm and aberrancies in the ventricular conducting system (left bundle branch block, left anterior fascicular block, left posterior fascicular block, widened QRS interval) [26]. Among the 1,400 patients studies, 79 had serious outcomes. Serious outcomes include death, myocardial infarction, arrhythmia, pulmonary embolism, stroke, subarachnoid hemorrhage, or significant hemorrhage. Table 4.Types of ambulatory monitoring devices Characteristics include duration that device is worn, whether the patient can trigger the device to record based on symptoms, whether the device records continuously or when a potential event is detected, whether the event strip is transmitted to the physician, and patient comfort/ease of performing their activities of daily living (ADLs). |
|
||||||||||||||||||||||||||||||||||||||||