INTRODUCTION
Renal colic is often observed among patients presenting to the emergency department and is one of the common causes of acute flank pain. Renal colic occurs in 3% to 5% of the population and develops most often in people aged 30 to 50 years [1]. Early diagnosis and appropriate treatment of ureteral stones are necessary to reduce their prevalence and facilitate an early return to activities of daily living. As larger stones obstruct natural excretion, the size of the ureteral stone is an important factor in decision-making in terms of treatment direction [2-4]. Hence, an accurate assessment of the maximum diameter of the ureteral stone is essential.
Ureteral stones can be round or elongated. Most elongated stones are vertically or longitudinally located. In a study that involved patients undergoing medical expulsive therapy, it was demonstrated that the longitudinal diameter of a stone was an important predictor of stone expulsion. It is therefore clinically important to always determine the size of a ureteral stone longitudinally [5]. Obtaining an accurate diagnosis is essential when patients are admitted to the emergency department with renal colic. Currently, non-contrast computed tomography (CT) is used to diagnose ureteral stones in patients with acute flank pain, and reportedly has almost 100% sensitivity and specificity [6-10]. Due to the recent use of multidirectional CT with enhanced resolution, clearer images can be obtained; moreover, coronal reconstruction CT enables the diagnosis of ureteral stone and assessment of its cross-sectional size with higher accuracy [11,12].
Although treatment guidelines, based on the size of the stone are well established (mainly horizontal diameter) [2-5], there are still only a few ongoing studies on the treatment guidelines in relation to the location and vertical diameter of the stone. There is a paucity of information on the relevant treatment options for ureteral stones based on their size and location.
Therefore, in the present study, we aimed to evaluate the influence of the location and size of the ureteral stones on the treatment option selection among urologists. In addition, we classified stones according to their locations (upper or lower ureter) and compared the differences in treatment according to the size of the stones at each location. The objective was to add to existing knowledge that would help urologists in selecting among treatment options in the emergency department.
METHODS
We retrospectively reviewed the medical records of adult patients (aged ≥18 years) with ureteral stones, admitted to the emergen cy department of a single medical center, between January 2009 and June 2014. We excluded patients aged <18 years, those with a history of a ureteral stone or kidney stone, those with multiple stones occurring bilaterally, those who were not followed up as outpatients, and those who did not undergo CT examination during admission. Institutional review board of Pusan National University Yangsan Hospital approval was obtained for the study (05-2015-103). The informed consent was waived.
Patient sex, age, history of ureteral stones, CT findings, and a type of treatment during outpatient follow-up were examined. In addition, the location of ureteral stones (upper or lower ureter) and the horizontal and longitudinal diameters of ureteral stones were measured using cross-sectional CT images and coronal reconstruction CT images, respectively
With regard to ureteral stone size, the horizontal diameter was defined as the largest diameter measured on cross-sectional CT, whereas the longitudinal diameter was defined as the largest diameter obtained via coronal reconstruction CT. The location of the stone was identified as the upper ureter (from the ureteropelvic junction to the ureter, crossing over the external iliac vessels) or the lower ureter (from the ureter crossing over the external iliac vessels to the ureterovesical junction). These were measured by a single emergency physician to reduce errors
Patients who underwent urologic intervention such as extracorporeal shock wave lithotripsy, ureteroscopy, and percutaneous nephrostomy were assigned to the urologic intervention group (group 1) and patients who underwent medical conservative therapy such as non-steroidal anti-inflammatory drugs, antispasmodics, α-antagonists, and fluid therapy were assigned to the medical treatment group (group 2). Patients diagnosed with ureteral stones in the emergency room returned home after pain management. The final decision regarding treatment was made by the urologist during the follow up period in the urologic outpatient clinic.
With regard to the primary results, the horizontal and longitudinal diameters of the ureteral stones were compared between groups. With regard to the secondary results, the location of ureteral stones in the ureter was determined. Moreover, the horizontal and longitudinal diameters of the stones were compared according to their location.
CT images were obtained via a 64-helical multidirectional CT system (Siemens Healthcare, Erlangen, Germany) and were viewed using the picture archiving and communicating system (Marosis; Infinite, Seoul, Korea).
Statistical analyses were performed using IBM SPSS Statistics ver. 23 (IBM Corp., Armonk, NY, USA). The t-test and the Mann-Whitney test were used for the analysis of continuous variables, whereas the chi-square test was used for the analysis of categorical variables. Decision-making with regard to treatment option, based on the horizontal and longitudinal diameters as well as the location of the stone, was investigated using the receiver-operating characteristic (ROC) curve, and the cut-off value, sensitivity, and specificity were compared. The ROC curve and the cut-off value were performed using the R program. A P-value of <0.05 was considered to indicate statistical significance.
RESULTS
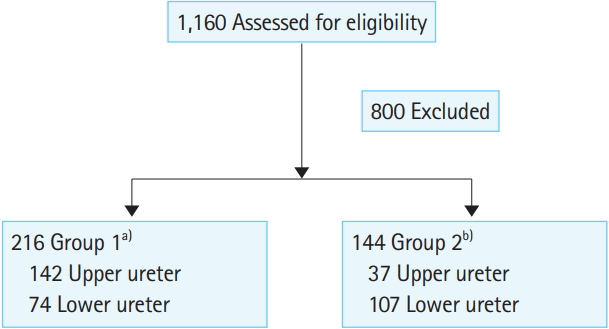
Herein, 1,160 patients were admitted and diagnosed with ureteral stones during the study period; of these, 360 were finally included in this study after excluding patients based on the exclusion criteria. Of these 360 patients, 238 (66.1%) were male and 122 (33.9%) were female. The mean age of patients was 50.5 ±13.6 years. An upper ureteral stone was detected in 179 patients (49.7%) and a lower ureteral stone was detected in 181 patients (50.3%). A total of 216 patients (60%) were assigned to group 1 and 144 patients (40%) were assigned to group 2. Based on the CT findings, the mean horizontal diameter of the ureteral stones was 5.4±3.9 mm, the mean longitudinal diameter of ureteral stones was 6.7±3.5 mm, and the mean ureteral diameter was 5.9±2.1 mm (Table 1 and Fig. 1).
The median values of the horizontal and longitudinal diameters (primary measurement results) were higher in the urologic intervention group than in the medical treatment group (median horizontal diameter: 5.5 mm [range, 4.8 to 6.8 mm] in group 1 and 4.0 mm [range, 3.0 to 4.6 mm] in group 2, P<0.001; median longitudinal diameter: 7.5 mm [range, 6.0 to 9.5 mm] in group 1 and 4.4 mm [range, 3.0 to 5.5 mm] in group 2, P<0.001). The differences were statistically significant in both groups (Table 2).
With regard to the location of the ureteral stone (secondary measurement results), 142 patients in the urologic intervention group and 37 patients in the medical treatment group had an upper ureteral stone, whereas 74 patients in the urologic intervention group and 107 patients in the medical treatment group had a lower ureteral stone. Urologic intervention was therefore, more common among patients with an upper ureteral stone (P<0.001) (Table 2).
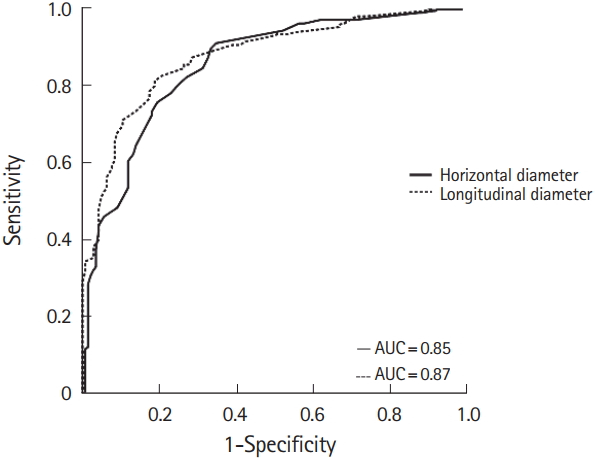
Based on a ROC curve analysis, the cut-off value for the horizontal stone diameter was found to be 4.75 mm, with a sensitivity of 80.6%, specificity of 75.5%, and area under curve (AUC) of 0.85 (95% confidence interval [CI], 0.82 to 0.94), whereas the cut-off value for the longitudinal stone diameter was found to be 5.65 mm, with a sensitivity of 81.3%, specificity of 81.5%, and AUC of 0.87 (95% CI, 0.83 to 0.91) (Fig. 2). This showed good discrimination.
ROC curve analysis conducted separately for the upper and lower ureteral stones showed the following results. For the upper ureteral stone diameter, the cut-off values were 4.45 and 6.25 mm, with sensitivities of 81.3% and 91.4%, specificities of 83% and 78.9%, and AUC of 0.88 (95% CI, 0.82 to 0.94) and 0.89 (95% CI, 0.83 to 0.93) for horizontal and longitudinal diameters, respectively. For the lower ureteral stone diameter, the cut-off values were 4.75 and 5.25 mm, with sensitivities of 79.4% and 79.4%, specificities of 76.3% and 73%, and AUC of 0.82 (95% CI, 0.75 to 0.88), 0.82 (95% CI, 0.75 to 0.88) according to the horizontal and longitudinal diameter, respectively. These showed good discrimination as well.
DISCUSSION
A decision regarding treatment option (whether to perform urologic intervention or medical treatment) is important for patients admitted to the emergency department who present with symptoms related to ureteral stones. A critical factor in choosing an optimal treatment option is the maximum diameter of a stone, which is inversely proportional to the probability of natural expulsion of the stone [2,3,13]. Urologic interventions such as extracorporeal shock wave lithotripsy, percutaneous nephrostomy, ureteroscopy, and open surgery can cause various complications including bleeding, puncture, injury to the kidney, and ureteral stenosis. The maximum diameter of the ureteral stone should therefore be used to guide decision-making with regard to primary treatment options and minimize the prevalence of complications [13,14].
Several studies have described the effectiveness of non-contrast CT and consider it as an optimal approach for the prompt diagnosis of patients admitted to the emergency department with renal colic [15-17]. Non-contrast CT images provide information on not only the location and size of the stone, but also, on internal indices such as the degree of ureteral stenosis, hydronephrosis, hydroureter, and inflammation around the kidney. As treatment options can differ based on variation in ureteral stone size by 1 to 2 mm, an accurate assessment of stone size is essential for obtaining vital information for treatment. A previous study has demonstrated that the horizontal diameter of a ureteral stone is smaller on cross-sectional CT images than on actual examination in 37% of cases [18], whereas another study has reported that the longitudinal diameter of the stone measured on cross-sectional CT images is larger than that measured via actual examination by 30% to 50% [19,20]. Hence, the longitudinal diameter of a ureteral stone measured using coronal reconstruction CT images can yield more accurate measurements and can aid in decision-making in terms of treatment option [18]; in fact, Lee et al. [5] indicated that the longitudinal stone diameter measured on coronal reconstruction CT images is a critical predictor of natural expulsion of stones.
Dalrymple et al. [21] reported that 77% of ureteral stones with a diameter of <5 mm, 60% of ureteral stones with a diameter between 5 and 7 mm, and only 39% of ureteral stones with a diameter >7 mm were naturally excreted; moreover, they found that urologic intervention was necessary for ureteral stones with a mean size of 6 mm, and that more than 80% of ureteral stones with a size of <4 mm were naturally excreted. Lee et al. [5] reported that more than 70% of upper and lower ureteral stones with a longitudinal diameter of <5 mm were naturally excreted, whereas less than 50% of upper and lower ureteral stones with a longitudinal diameter of >5 mm were naturally excreted. Similar findings were observed in the present study (Table 2). Only medical conservative treatment was performed if the horizontal and longitudinal diameters of ureteral stones and the ureteral diameter were <5 mm, whereas urologic intervention was more likely if these values were >5 mm. Moreover, Fig. 1 shows that urologic intervention was more likely if the horizontal stone diameter was >4.75 mm (sensitivity 80.6%, specificity 75.5%) and the longitudinal diameter was >5.65 mm (sensitivity 81.3%, specificity 81%).
Stone location is also an important factor. Anatomically, the ureteropelvic junction, the portion of the ureter that crosses over the external iliac vessels, and the ureterovesical junction are known to be narrow and can easily be blocked [22]. A previous study reported that 35.7% of ureteral stones were located in the upper ureter and 63.1% were located in the lower ureter; moreover, a reduced distance between the stone and the ureterovesical junction was associated with a smaller stone size, and the stones located in the ureterovesical junction were most often naturally excreted, as compared to stones located in other locations [23]. However, in the present study, an equivalent number of patients exhibited stones in the upper ureter (49.7%) and in the lower ureter (50.3%), and the patients with upper ureteral stones were more likely to undergo urologic intervention. Eisner et al. [22] reported that upper ureteral stones had larger horizontal and longitudinal diameters than lower ureteral stones; however, the findings of the present study differed from those of the study of the Eisner et al. [22] in that the horizontal diameter was larger for lower ureteral stones and the longitudinal diameter was larger for upper ureteral stones. As shown in Fig. 2, patients with upper ureteral stones were more likely to undergo urologic intervention if the horizontal stone diameter was >4.45 mm (sensitivity 81.3%, specificity 83%) and longitudinal stone diameter was >6.25 mm (sensitivity 91.4%, specificity 78.9%), and patients with lower ureteral stones were more likely to undergo urologic intervention if the horizontal stone diameter was >4.75 mm (sensitivity 79.4%, specificity 76.3%) and the longitudinal stone diameter was >5.25 mm (sensitivity 79.4%, specificity 73%). In addition, stones with a larger longitudinal diameter were more likely to be located in the upper ureter than in the lower ureter, making natural excretion of these stones more difficult. In conclusion, the longitudinal diameter is a critical factor in deciding whether or not urologic intervention is necessary.
The available options for treating ureteral stones include conservative therapy such as anti-inflammatory analgesics, α-antagonists, and fluid therapy or urologic interventions such as extracorporeal shock wave lithotripsy, percutaneous nephrostomy, and ureteroscopy. With regard to the treatment option, it is important to identify the location, size, and shape of the stone in order to decide on an appropriate treatment method [23]. Most ureteral stones with a diameter of <5 mm are naturally excreted within 4 weeks, and hence, treatment may only involve observation and management of symptoms such as pain in these cases [1,3]. In contrast, the stones with a diameter of >10 mm require urologic interventions such as extracorporeal shock wave lithotripsy, ureteroscopy, and percutaneous nephrostomy [13].
The present study has certain limitations. First, as the study was retrospectively conducted on patients from a single hospital, the findings cannot be generalized; a prospective multi-institute study will be needed in the future. Secondly, stone size was measured by a single individual, and hence, there may be some measurement bias. In addition, factors that affect urologic intervention (age; underlying disease; hematologic, urinary, and stool test findings; disease history) were not considered, and the study was conducted by mainly focusing on the size and location of ureteral stones, which could have produced bias. Fourth, we were unable to determine the treatments for patients who were not followed up as outpatients. Typically, the patients who are not followed up on as outpatients have a mild condition; their exclusion from the study may have influenced the study findings. Last but not least, since this study was retrospective in nature, we could not monitor the natural expulsion of stones. Therefore, the treatment was determined by the subjective judgment of the urologist without sufficient follow-up observation. This subjective view could result in errors.
The probability of receiving urologic intervention was higher for patients who had upper ureteral stones, as wells as for cases whose stone diameter exceeded 5 mm horizontally, and 6 mm longitudinally. The treatment option is determined by the location and size of the stone, as well as the measurement dimension (whether horizontal or longitudinal).