INTRODUCTION
Post cardiac arrest brain injuries are characterized by severe global anoxic ischemia, followed by reperfusion injury cascades [1]. Many cardiac arrest survivors have low survival rates and a high rate of poor neurologic outcomes, despite advances in post cardiac arrest critical care, including temperature management [2]. Targeted temperature management (TTM) has been thought to be beneficial for patients as hypothermia affects pathways leading to apoptosis, inflammation, and free radical production, as well as blood flow and metabolism throughout the acute, subacute, and chronic stages of reperfusion injury ongoing for several days [1].
Many experimental studies have investigated hemodynamic and metabolic changes in brain physiology with a temperature change during hypothermia and rewarming phases [3,4], reporting risk of brain edema and increased intracranial pressure (ICP), along with changes in cerebral blood flow during the rewarming phase [5-7]. The current guidelines, based on major multicenter randomized controlled trial studies [8-10], recommend rewarming patients after targeted temperature hypothermia at a rate of 0.25°C/hr to 0.5°C/hr [11]. Slower rewarming rates may be beneficial by reducing myocardial injury, cerebral injury, and inflammatory reactions as shown in an animal study [12]. Further, slower rewarming rates are used in other brain injury etiologies with a similar ischemic-reperfusion injury, such as ischemic stroke [13]. However, the optimal rewarming rate is unknown as clinical studies investigating rewarming rates and patient outcomes are lacking. This pilot study is the first to investigate the neurologic outcomes of post cardiac arrest patients who were rewarmed at the rates of 0.15°C/hr and 0.25°C/hr after 24 hours of hypothermia.
METHODS
This study was approved by the institutional review board of Ajou University Medical Center (MED-MDB-17-282). Requirement of informed consent was waived owing to its retrospective nature.
Study design and population
This retrospective cohort study included adult patients who underwent TTM after out-of-hospital cardiac arrest or cardiac arrest in the emergency room and were admitted to the intensive care unit for post cardiac arrest care between January 2016 and August 2017. Patients with pre-existing diseases such as terminal cancer with a life expectancy of less than 6 months, and those with a do-not-resuscitate order with request from the family did not undergo TTM. The exclusion criteria of this study were as follows: 1) deceased status before the rewarming phase as it would be difficult to determine the effect of the rewarming rate; 2) earlier-than-planned rewarming with a change in the target temperature or discontinued TTM due to unstable hemodynamic status; 3) target temperature of 35°C or 36°C because the effect of the rewarming rate cannot be assessed; and 4) rewarming not as planned, owing to TTM methods using a device without a feedback loop system.
Data collection
The data were retrospectively retrieved from the post cardiac arrest TTM database and electronic medical records. Demographic data, including age and sex, and cardiopulmonary resuscitation (CPR) data, such as arrest time and location of arrest; initial rhythm; underlying disease; hypothermia data, such as method of hypothermia, target temperature, and duration of hypothermia; rewarming rate; and patient outcomes expressed as the cerebral performance category (CPC) score, were obtained from the registry. The arrest time was defined as the sum of the duration of CPR, both prehospital and in the hospital. The neurologic outcome, which was the primary outcome of this study, was assessed using the CPC score after 1 month. Good neurologic outcome was defined as a CPC score of 1, 2 and poor neurologic outcome as a CPC score of 3 to 5. Incidence of pneumonia during or after the rewarming period was reviewed by investigating electronic medical records and the formal chest x-ray report by radiologists.
Study setting and TTM protocol
The institute is a tertiary academic hospital with an annual emergency department visit number of approximately 87,000 patients. The post cardiac arrest protocol recommends a target temperature of 33°C unless the patient is hemodynamically unstable or has a bleeding tendency or severe infection. Two attending physicians (A and B) decided the treatment plan for the post cardiac arrest patients. Since 2016, physician A changed the rewarming rate to 0.15°C/hr when on duty, after occasionally observing deterioration of brain stem reflexes during the rewarming phase, while physician B continued to rewarm at a rate of 0.25°C/hr. Physicians A and B were on duty attending for the same amount of time, alternating every 2 months. All other treatment was performed using a strict post cardiac arrest protocol. TTM was conducted with the use of temperature managing devices with a feedback loop system (Artic Sun Energy Transfer Pads, Medivance Corp., Louisville, CO, USA; Cool Guard Alsius Icy Heat Exchange Catheter, Alsius Corporation, Irvine, CA, USA). All patients had sufficient sedation and analgesia for shivering control and seizure control, if needed.
Statistical analysis
Continuous variables were expressed as means and standard deviations or medians and interquartile ranges depending on normal distribution. Categorical variables were expressed as number and. The researchers used the chi-square test or Fisher exact test for nominal variables and the t-test or Mann-Whitney U-test for continuous variables. The researchers performed logistic regression analysis to determine if the rewarming rate was associated with the neurologic outcomes and mortality. A univariate analysis was performed prior to the multivariate analysis, and a backward selection of variables was used to determine variables to be included in the multivariate logistic regression model. P<0.05 was considered statistically significant. The researchers used Stata ver. 14.0 (StataCorp., College Station, TX, USA) for the statistical analysis.
RESULTS
Characteristics of the study subjects
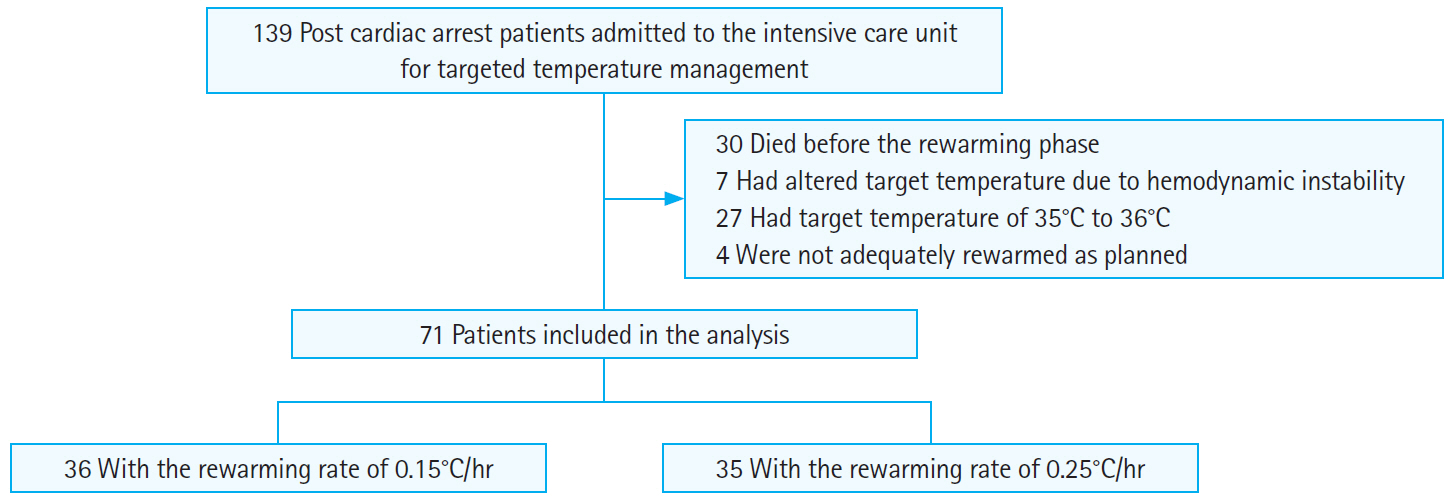
Among the 139 cardiac arrest survivors who were admitted to the intensive care unit for post cardiac arrest care, 30 patients died before the rewarming phase. Seven patients had a change in the target temperature due to hemodynamic instability; 27 patients had a target temperature of 35°C or 36°C; and 4 patients were not adequately rewarmed as planned owing to temperature managing methods without a feedback loop. A total of 71 patients were analyzed, including 36 patients rewarmed at a rate of 0.15°C/hr and 35 patients rewarmed at a rate of 0.25°C/hr, after a 24-hour duration at target temperature (Fig. 1). The baseline characteristics are shown in Table 1. All variables, including demographics, arrest characteristics, and outcomes, such as survival to discharge and neurologic outcomes, did not significantly differ between the groups rewarmed at the rates of 0.15°C/hr and 0.25°C/hr. This study also investigated the incidence of pneumonia based on the two rewarming rates; the frequency did not significantly differ.
Rewarming rate and outcomes
The association of the rewarming rate with the neurologic outcomes is shown in Table 2. The rewarming rate of 0.15°C/hr was not associated with the neurologic outcomes after 1 month in the univariate analysis (odds ratio, 0.96; 95% confidence interval, 0.41 to 2.26; P=0.92). Even after adjusting for confounding factors, such as age, sex, witnessed arrest, presumed cardiogenic cause, and CPR duration the rewarming rate of 0.15°C/hr was still not associated with the neurologic outcomes (odds ratio, 0.54; 95% confidence interval, 0.16 to 1.69; P=0.28).
DISCUSSION
This study aimed to investigate whether the different rewarming rates of 0.15°C/hr and 0.25°C/hr were associated with the neurologic outcomes in post cardiac arrest patients who underwent TTM. Although the study was limited by its small number of patients, the rewarming rate of 0.15°C/hr was not found to be associated with improved neurologic outcomes in this pilot study.
TTM is thought to be beneficial in post cardiac arrest patients by decreasing cerebral metabolism, free radical production, and proinflammatory cytokines, as well as intracranial pressure [14,15]. However, after maintenance of hypothermia at the target temperature, changes in cerebral hemodynamics and metabolism may occur during the rewarming phase [16,17]. Previous studies, including studies on patients undergoing cardiac bypass surgery or other brain injury etiologies, such as trauma, have shown that increased ICP, incidence of cerebral injury, and metabolic rate can occur during the rewarming period; further, rapid rewarming may be associated with worse cognitive outcomes [5,18], and slow rewarming showed better cerebral oxygenation as monitored by jugular bulb saturation or near-infrared spectroscopy [19]. Furthermore, the study by Naito et al. [7] on post cardiac arrest patients with ICP monitoring reported a major ICP increment during the rewarming period. Although the guidelines suggest a rewarming rate of 0.25°C/hr to 0.5°C/hr for TTM [11], evidence to support the optimal rewarming rate is lacking.
The study by Bouwes et al. [20] showed a tendency to poor neurologic outcome in post cardiac arrest patients when the rewarming rate was faster than 0.5°C/hr. Another study on post cardiac arrest patients investigated favorable neurologic outcomes based on different target temperatures and rewarming duration protocols (<28 vs. ≥28 hr) and failed to find significant differences in the outcomes (35% vs. 41%, P=0.39) [21]. This study also showed that the difference in the rewarming rates of 0.15°C/hr and 0.25°C/hr was not associated with the neurologic outcomes.
A major limitation was the small number of patients included in this study. The estimated sample size for this study from a previous observational study with a sufficient power was 220 patients [20]. However, since we started rewarming at a rate of 0.15°C/hr in 2016, we could not gather enough subjects. In addition, we excluded patients with high target temperatures that may mask the effect of rewarming rate and patients with early rewarming due to hemodynamic instability, so the sample size was limited. This was the first single-center pilot study that investigated these rewarming rates, and the authors acknowledge that there is a risk of a type II error; further studies are needed with more patients for sufficient power before confirmation of the results. A sample size calculation based on the results of this study required 3036 patients for an alpha error of 0.05 and power of 80%. Another limitation of this study is the retrospective design from the data collected from a single tertiary center. This may limit the generalizability of the findings. Moreover, the rewarming rate was selected by the attending physician on duty. Although the rest of the post cardiac treatment was performed by protocol, there may be other uncounted preferences in patient treatment between physicians A and B, which might have affected the results of the study. Selection bias may have occurred by selecting different rewarming rates depending on the patient condition. However, when physician A was on duty, the default rewarming rate was 0.15°C/hr unless the patient was unstable and required earlier rewarming. Further, patients whose target temperature or rewarming rate due to instability had to be altered were excluded from the study. Therefore, the rewarming rates were generally decided by the physician who was on duty rather than patient conditions. Although the baseline characteristics were similar, there may be other confounding variables, which might have affected the findings of this study. Future larger studies that would investigate optimal rewarming rates with a prospective randomized design are needed.
In summary, the findings of this study suggest that the rewarming rates of 0.15°C/hr and 0.25°C/hr after 24 hours of targeted hypothermia may not be associated with a difference in the neurologic outcomes among post cardiac arrest patients. However, as the number of patients included was limited, further studies are needed to determine the optimal rewarming rate.