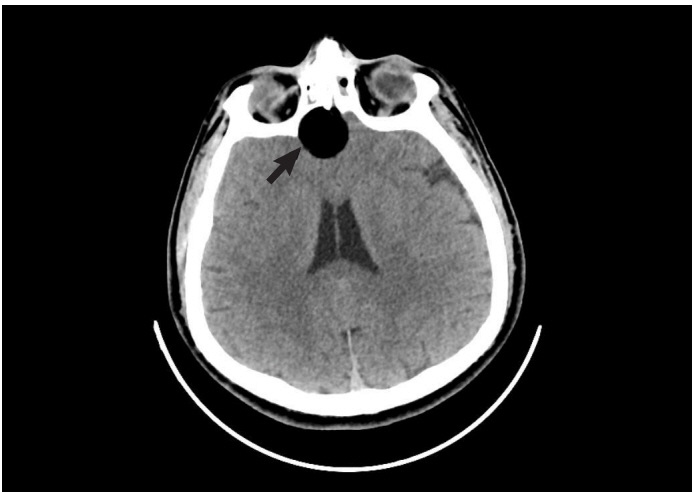
A 40-year-old male was admitted to the emergency department with syncope after a tonicclonic seizure and urinary incontinence. His relatives reported that he had remained asleep for approximately 10 minutes after seizing. There was no past medical history or drug use. On admission, his vital signs, blood glucose level, and neurological examination were normal. He had a Glasgow coma score of 15 and was oriented and cooperative. Systemic physical examination revealed no abnormalities. Computed tomography imaging was performed to rule out intracranial pathologies that showed a 16×22-mm diameter solid fat density lesion in the frontal lobe, and fat droplets in the subarachnoid space consistent with rupture (Figs. 1, 2). Surgical intervention was performed by the neurosurgeon and postoperative improvement was seen without sequelae.
Dermoid cysts originate from the ectopic inclusion of epithelial cells during neural tube closure in embryonic development [1]. They are usually non-malignant lesions that occur in midline, sellar, parasellar, and frontonasal regions, which are asymptomatic until rupture or infection [2]. Rupture is generally spontaneous, but in some cases, can occur due to head trauma or surgery [3]. The clinical symptoms of acute rupture include headache, nausea, vomiting, vertigo, vision problems, aseptic chemical meningitis, hemiplegia, hydrocephalus, vasospasm, cerebral ischemia, mental changes, and coma [4]. Computed tomography is the initial imaging method used in emergency departments. On computed tomography, these lesions have internal density characteristics consistent with fat (Hounsfield unit, -20 to -140) [4]. Dermoid cysts should be considered as a differential diagnosis of seizure that is easily recognized using conventional imaging methods.