INTRODUCTION
The maturation of emergency medicine as a specialty has coincided with dramatic increases in emergency department (ED) visit rates worldwide [1]. Patients who present to EDs often face long wait times for treatment; moreover, those who require admission wait even longer for an inpatient hospital bed [2]. ED timeliness is a critical factor affecting the operational performance of the complex processes required to deliver emergency care. Operational performance ultimately affects the quality of care, patient safety, and operational and financial efficiency [3]. Many interventions to manage ED crowding have been implemented in order to improve the efficiency of ED operation by eliminating waste, reducing variability, and increasing flexibility [4,5]. The problem remains despite these efforts, because ED crowding is not only a problem related with individual EDs, but is rather a reflection of a larger supply and demand mismatch in the healthcare system [2].
In the conceptual model of the ED, previous interventions mainly target throughput and output components. ED supply systems concerning patient care processes and patient disposition are manageable; however, the input component, which includes any condition, event, or system characteristic that contributes to the demand for ED services, is not easily reducible or predictable [2]. Ambulance diversion to other EDs or telephone triage services to reduce ED demand have limited effects on the overall emergency medical system [3]. Furthermore, ED demand at a given time appears impossible to predict, and there is a lack of analytic research. The input component usually predicts the average ED patient volume over a certain period, despite the lack of evidence indicating that the average is adequately representative of the variability of ED patient visits [6-8].
Efficient operation requires individual EDs to estimate how many busy days will occur and can be reduced with additional medical resources as well as how often “on-call” resources will be needed. Thus, hourly ED visit data should be collected and processed to address these questions. Accordingly, processed nationwide ED visit data could be used to construct a road map to develop policies for the entire healthcare system from the perspective of the expanded input-throughput-output conceptual model [9]. Thus, the present study evaluated the daily variability in hourly ED visit volume.
METHODS
Study design and primary outcome
This was a retrospective observational study that aimed to characterize the daily variability of hourly ED visits and evaluate the representativeness of the average. We created and analyzed 24 bar graphs in a histogram of the average hourly ED visit volumes over 365 days as well as 24 box-plots of hourly ED visit volume over 365 days.
We analyzed the nationwide ED patient visit time data of the National Emergency Medical Center not only to provide information about a particular ED, but also to evaluate EDs in general. Since 2004, the National Emergency Medical Center in Korea has collected standard ED visit patient data including time of visit, sex, age, chief complaint, result of disposition, route of visit, vital signs, and date and time of discharge from nationwide EDs via an automated reporting system, the National Emergency Department Information System (NEDIS); it offers these data as a text file containing the times of visit of nationwide EDs in 2013 [10].
Data analysis
The ED visit patient data were divided into 24 hours and 365 days according to visit time, and a 365×24 data table was constructed. The 8,760 values in the resultant data table were analyzed by descriptive statistics to create bar graphs showing the means and 95% confidence intervals as well as box plots to present the hourly and daily characteristics of ED visit variability for comparison with the bar graphs. For the statistical analysis of the representativeness of the means, the Shapiro-Wilk test was performed to test the normality of the distribution of the hourly ED visit volume over 365 days; skewness and kurtosis were also calculated.
The text file including ED visit time data were collected and converted to comma separated value format by using Microsoft Excel 2010 (Microsoft Corp., Redmond, WA, USA). The graphs were created and statistical analysis was performed by using R version 3.1.3 developed by the R Foundation for Statistical Computing (R Development Core Team, 2005, http://www.R-project.org). The study protocol and exemption from informed consent were approved by the institutional review board of the Jeju national University Hospital.
RESULTS
In 2013, the NEDIS annual report stated 4,919,181 patients visited 141 EDs in 16 provinces nationwide (Table 1) [10]. However, as the information transmission rate to the NEDIS was approximately 94%, the available text file contained the arrival times of 4,672,275 patients in 2013 [10].
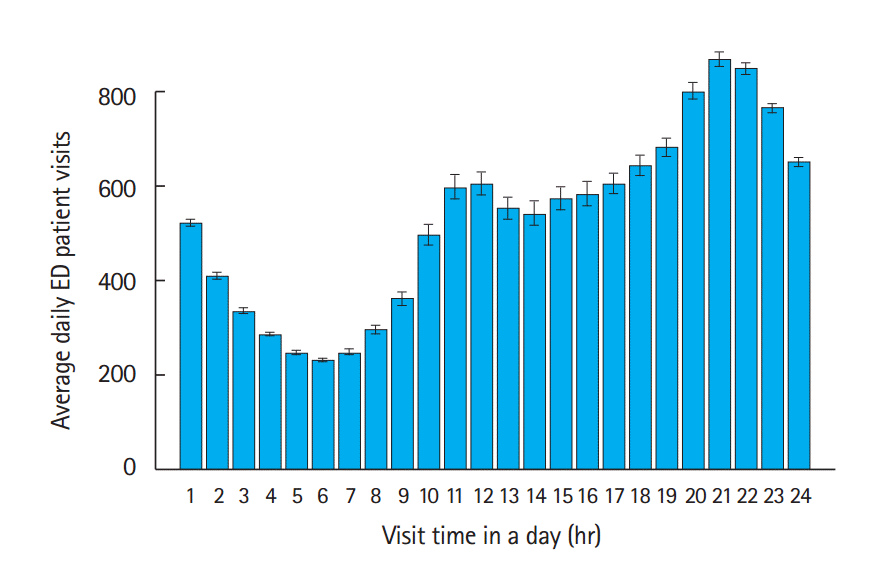
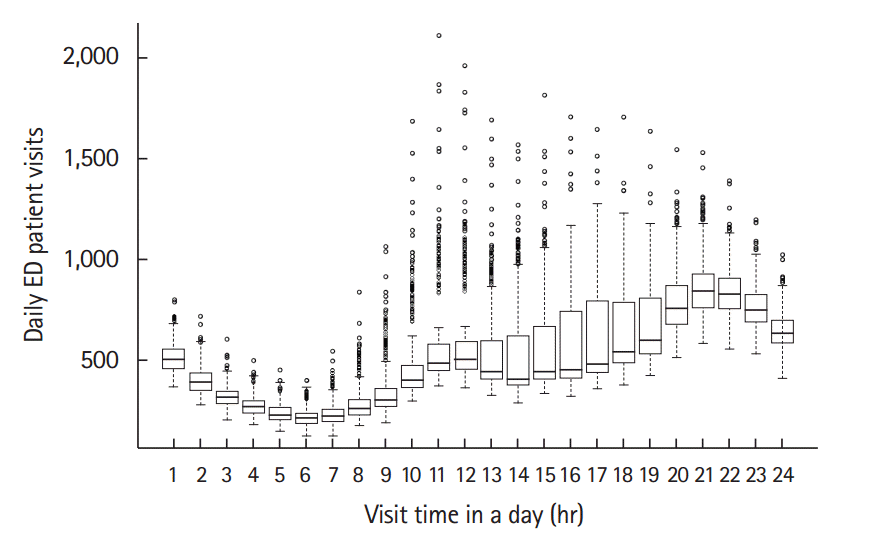
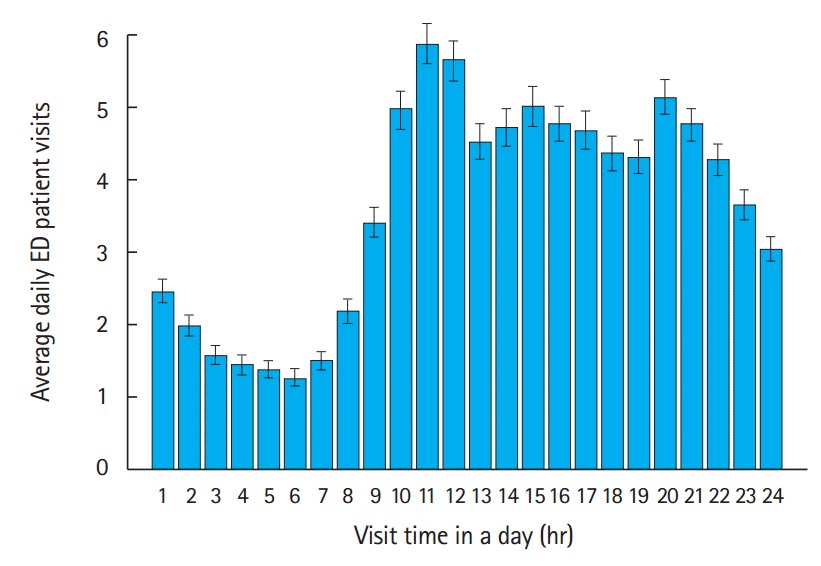
The bar graphs and box plots of EDs nationwide are shown in Figs. 1 and 2, respectively. The hourly visit pattern in one day showed a bimodal distribution with peaks from 10:00 to 11:00 and 20:00 to 21:00. The period with the lowest visits was 02:00 to 08:00. The box plots (Fig. 2) of the ED visit volume at each time showed upside-skewed interquartile ranges rather than a symmetric distribution in addition to the median volume.
DISCUSSION
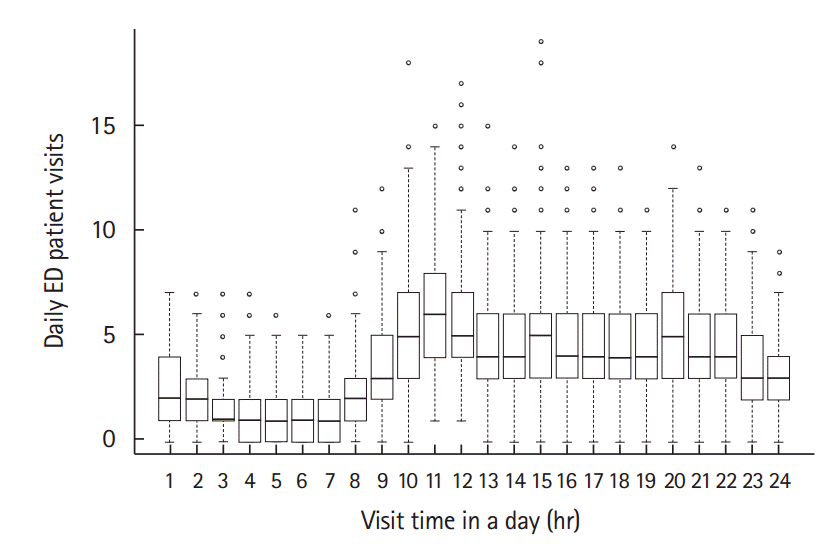
The bimodal feature of the average hourly ED patient visit volumes identified in the present study is similar to the findings of previous studies [11,12]. The authors of those studies assumed there was no significant variability in visits over 365 days at a given time of day; therefore, the average was used as the representative value. However, the box plots showed positively skewed and widely dispersed distributions of visit times and this causes the more-frequent “low visit volume days” to decrease the average, consequently masking the less-frequent “high visit volume days.” In the case of a given ED with a visit volume similar to that shown in Fig. 4 (with a volume difference of approximately 1.6 patients per hour between the 1st quartile and average), an ED operator who prepares the ED expecting the average ED visit volume may experience 1.6 more patients per hour in three months (25%) in a given year. Unfortunately, the unbounded positive range also indicates that ED crowding cannot be completely prevented in cases such as disasters. Therefore, “permissive busy ED days” should be determined in order to prevent excessive waste of medical resources. Accordingly, further simulation studies will allow us to predict how much more medical resources might be needed to reduce the number of busy days below a particular percent in a year.
The features of the box plots presented herein may differ from those of other emergency medical systems with different socioeconomic situations and emergency medical service utilization habits. Furthermore, as patient visit volumes can change over time, the annual change should be taken into consideration [1]. Nevertheless, the box plots verify the daily variability of ED visit volumes.