INTRODUCTION
On January 26, 2015, the Ministry of Health and Welfare reorganized existing emergency medical care based on urban centers rather than municipalities. The Ministry also announced preliminary public notification of the provisions of the partial amendment to the Enforcement Regulations of the Act of Emergency Medical Care, which was intended for the designation of additional urban centers for emergency medical care [1]. The principal provisions of this amendment notification are to provide active emergency medical care services by designating additional urban centers for emergency medical care. These provisions also mandate five or more emergency medicine (EM) specialists, such that at least one specialist is present in the emergency department at all times in order to improve emergency patient survival rates [1]. This mandate reflects the reality of increasing utilization of emergency departments, which have unlimited outpatient service hours and relatively high accessibility. During the medical professional labor strike in June 2000, specialists were temporarily in charge of primary care for patients visiting emergency departments. Thereafter, some reports showed encouraging results of primary care medical services provided by specialists in charge of emergency departments [2-4], which resulted in reduced use of unnecessary patient tests based on the specialists’ (1) abundant experience, (2) knowledge, (3) duration of care making admission decisions for patients, and (4) amicable mutual collaboration with other departments. This resulted in decreased duration of emergency department stays as well as reduced rates of non-emergency patient admissions. A comprehensive survey of EM specialists conducted in 2010 predicted that a total of 1,505 to 2,270 EM specialists would be necessary in order to have at least one EM specialist to care for all patients visiting each emergency department per each working hour [4-6]. However, a total of 1,211 board-certified EM specialists are reportedly working in EDs in 2015. This number is insufficient for the number of patients visiting emergency departments in Korea [4]. In an effort to investigate the most efficient measures to utilize the limited number of EM specialists, this study divided patients who visited the emergency department of a tertiary care general hospital into two groups: the SS group, in which patients were supervised by an EM specialist; and the SOC group, in which patients were supervised by an EM resident with an EM specialist on call. Differences in mortality rates by severity and duration of stay in the emergency department were compared between these two groups. This analysis may help in establishing the duty and the role of EM specialists and inform relevant policy making.
METHODS
Data source
This study included adult patients who visited the emergency department of a tertiary care general hospital in Seoul from March 1 to December 31, 2012. Patients aged 15 years or less, pregnant women presenting for delivery, patients declared dead on arrival, and patients with cancelled admittance were excluded.
Subject setting
Subjects were divided into two groups: the experimental, specialist-supervised (SS) group with four or more EM specialists who regularly made clinical decisions for visiting patients from 9 a.m. to 5 p.m.; and the control, specialist-on-call (SOC) group, in which a senior EM resident made clinical decisions for visiting patients and a EM specialist was placed on call as needed from 5 p.m. to 9 a.m. the next morning. In this study, an EM specialist was defined as a board-certified specialist who had completed a resident training program. A senior EM resident was defined as a third or fourth-year resident in an EM resident training program. Clinical decisions were verified by review of initial examination, clinical course, and discharge records from electronic medical records.
Data collection
This study was approved by the institutional review board. Electronic medical records used in the emergency department at the time of medical care were retrospectively investigated.
Outcome measures
Patients visiting the emergency department were investigated with respect to age, sex, time presenting to the emergency department, severity of condition finally classified during the emergency department visit, main symptoms, principal diagnosis, department of medical care, main clinical department, duration of direct patient consultation performed by an EM physician during visit, length of time for requesting on-call physician from another department, clinical outcome (discharged, transferred, admitted, and died), and length of stay in the emergency department. Mortality was estimated based on the time elapsed from admission to ED, not on the time of death.
Severity scale
The general hospital in which this study was conducted is a tertiary care center with more than 100,000 patient visits to the emergency department each year. EM specialists or nurses with at least five years of clinical experience classified the severity of all visiting patients using the modified Canadian Triage and Acuity Scale (CTAS), autonomously complemented from the comprehensive 5-level classification of the CTAS. The CTAS levels classify the severity of patient conditions from level 1 to level 5 based on past medical history and clinical findings on arrival at the emergency department. Level 1 represents the sickest patients, while level 5 represents the least ill patients. The modified CTAS is a partially revised acuity scale tool that reduces the interval between assessments, and classifies trauma cases as a more severe level.
Statistical analysis
PASW Statistics ver. 18.0 (SPSS Inc., Chicago, IL, USA) was used for statistical analysis of data. Chi-square and student’s t-tests were used for comparison of categorical and continuous variables, respectively. Kaplan-Meier survival analysis was used to determine accumulated mortality rates and hazard ratios. P-values less than 0.05 were considered statistically significant. The numbers from study results were rounded off to two decimal digits.
RESULTS
Demographics
The general characteristics of subjects were as follows: the SS group contained a total of 25,747 patients, including 13,247 men (51.5%) and 12,500 women (48.5%). The SOC group contained 28,457 patients, including 14,153 men (49.7%) and 14,304 women (50.3%). The gender ratio differed significantly between the two groups (P<0.05). There was also a significant difference in clinical outcome between groups (P<0.05). The largest proportion of cases in the SS group were discharged (15,473 patients, 60.1%), followed by ward admission (8,981 patients, 34.9%), transfer to another hospital (1,238 patients, 4.8%), and death (55 patients, 0.2%). Similarly, the largest proportion of cases in the SOC group was discharged (20,283 patients, 71.3%). There was a significant difference between groups with respect to severity (P<0.05). The numbers of patients classified as having mild illness (levels 4 and 5) in the SS and SOC group were 18,611 (72.3%) and 21,462 (75.4%), respectively (Table 1). Table 1 shows that most patients visiting the emergency department were classified as having conditions of mild severity (Table 1).
Consultation with outside departments
An internal medicine consult was requested for 10,423 (19.2%) patients in the SS group, followed by EM (9,100, 16.8%) and general surgery (1,767, 3.3%) consultations. In contrast, the largest proportion of consult requests in the SOC group were to EM (14,106 patients, 26.0%), followed by internal medicine (7,761, 14.3%) and general surgery (1,593, 2.9%). The rate of consultations differed significantly between the two groups (P<0.05) (Table 2).
Mean length of emergency department stay, elapsed time to EM physician visit, and time to consult another department
The mean length of emergency room stay in the SS group was 864.09±1,101.88 minutes, while that of the SOC group was 613.71±922.37 minutes, a significant difference between groups (P<0.05). The mean elapsed time for an EM physician to visit a patient after arrival (EM visit to patient time) in the SS group was 18.86±18.36 minutes, while that of the SOC group was 16.37±16.43 minutes, a significant difference between groups (P<0.05). The mean durations before requesting consults from another department (consult time) in the SS and SOC groups were 23.22±110.39 and 17.39±93.79 minutes, a significant difference (P< 0.05) (Table 3).
Differences in emergency department length of stay according to severity levels
There were differences in length of stay in emergency department according to severity level in the SS group (P<0.05). The mean length of stay of patients with severe-to-moderately severe conditions (levels 1 to 3) in the SS group was 1,189.15±1,208.69 minutes, while that of the SOC group was 1,050.99±1,108.37 minutes, a significant difference (P<0.05). The mean length of stay in the SS group was longer than that of the SOC group. The mean length of stay of patients with mildly severe conditions (levels 4 and 5) in the SS group was 739.45±1,031.29 minutes, compared to 471.18±803.17 minutes in the SOC group, a significant difference (P<0.05). The mean length of stay of the SS group was longer than that of the SOC group (Table 4).
Survival analysis of patients with severe-to-moderately severe conditions (levels 1 to 3)
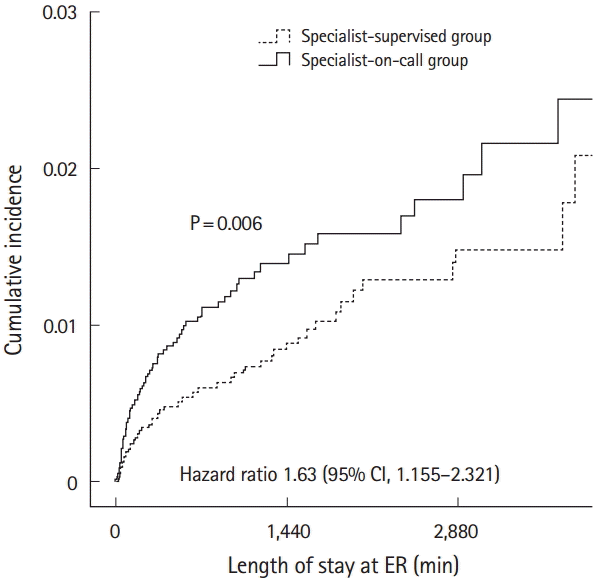
Kaplan-Meier survival analysis was used to determine the hazard ratios of patients in the SS and SOC groups with moderate-to-severe conditions (levels 1 to 3). The hazard ratio was 1.637 (95% confidence interval, 1.155 to 2.321), indicating a 63.7% higher hazard for patients in the SOC group than that of the SS group. The results of survival analysis showed a significant difference between the two groups. Significant differences were also observed in the analysis of survival rates performed to validate the differences between groups (P<0.05). In other words, the survival rate of patients in the SS group was higher than that of patients in the SOC group. Furthermore, the accumulated mortality rate decreased due to the increased length of stay in the emergency department. This significant difference (P<0.05) is shown in Fig. 1.
DISCUSSION
Medical care of patients visiting emergency departments has traditionally been the territory of relatively inexperienced medical interns in Korea. Interns are typically supervised by residents or specialists, linking through inter-disciplinary consultations as required [7,8].
However, primary examinations and diagnoses performed by relatively inexperienced doctors may result in delays in timely and proper treatment of patients requiring urgent management. This delay may result in disputes with patients and guardians regarding medical expenses and increased length of stay for unnecessary tests. The number of patients visiting emergency departments has increased 6% every year, reflecting the increasing role and importance of medical services offered by emergency departments. Annually, about 150 EM specialists are board-certified, but these numbers are not enough to meet the rising demand due to increasing numbers of patients. Thus, to reduce length of stay for patients visiting the emergency department and increase satisfaction, there is an increasing demand for EM specialists in emergency departments to provide rational and professional emergency care. During the nationwide doctors’ strike regarding the separation of prescribing and dispensing of drugs in 2000, specialists provided round-the-clock medical services in hospital emergency departments for approximately six months. The services provided by specialists in the emergency department relatively decreased patient length of stay while not negatively affecting mortality rates. The specialists reduced the number of unnecessary tests and increased patient satisfaction, as reported by various studies [2,3,9]. Furthermore, an acuity scale tool was used to triage patients and provide rational management of emergency departments [10]. Medical services provided by EM specialists to patients with mildly severe conditions decreased waiting time and length of stay in emergency departments compared to groups without EM specialists. The medical services provided by EM specialists also increased patient satisfaction [11-13]. The current study divided subjects into two groups: the SS group, in which an EM specialist supervised patients’ medical care; the SOC group, in which an EM resident supervised medical care with an EM specialist on call, in order to perform comparative analyses. There was a difference in clinical outcome and acuity scale between the two groups. The number of patients with mildly severe conditions (levels 4 and 5) was greater between 5 p.m. and 9 a.m. of the next day, when one or more EM specialists provided emergency services, as opposed to 9 a.m. to 5 p.m. when four or more EM specialists were available to render services. Thus, this observation was expected as a result of increased numbers of discharge cases as determined by clinical outcome. The rate of consultation requests from on-call physicians in the department of internal medicine was highest in the SS group, while the rate was highest for EM physicians in the SOC group. The high consult rate was affected by patients transferred from the outpatient department of internal medicine who were admitted to the hospital through the emergency department during the regular hours, when four or more EM specialists were available. Patients may be admitted through the hospital, clinics, and outpatient departments during regular hours. Thus, the proportion of patients with mildly severe conditions was relatively lower in the department of EM. Moreover, the duration of stay in the emergency department and the length of time to request consult from other departments relatively increased when an EM specialist was involved with the clinical decisions. The number of tests performed and the length of stay increased in the emergency department in order to provide accurate diagnosis and treatment; additional tests such as computed tomography or magnetic resonance imaging might be delayed in overcrowded emergency departments. Patient care performed by an EM specialist leads to such results. However, it is difficult to make simple comparisons, since other factors such as differences in the numbers of patients cared for by EM specialists and EM residents, differences in available tests depending on the time of day, and differences in length of time required to perform duties other than medical services.
Relative to the length of stay, the mortality rate was significantly lower in the group of patients with severe-to-moderate conditions (levels 1 to 3) supervised by an EM specialist who made clinical decisions.
Efficient utilization of manpower is possible by assigning the relatively limited number of EM specialists to supervise patients with severe-to-moderate illness (levels 1 to 3, the group with the highest mortality rates), while senior EM residents supervise patients with mild illness (levels 4 and 5), with an EM specialist on call as needed.
This study has several limitations. First, we analyzed data from a single tertiary-care general hospital. Thus, the findings may not be applicable to other institutions since the work conditions, intensity, and EM specialist hours differ at each hospital. Second, because the patients were classified into groups based on the working hours of EM specialists, various intervening factors, including differences between day and night shifts, types of applicable tests, and supportive divisions, could also have affected the observed results. However, these factors likely had a limited effect on the results of this study due to (1) the nature of EDs, in which emergency medical services are provided 24 hours a day, seven days a week, and (2) there was no difference in the severity rates of patients between the two groups. Further prospective, multicentered studies could better elucidate the role of EM specialists in the ED. Third, the retrospective study of this investigation prevented assessment of the effects of the clinical decisions and care provided by EM specialists on the qualitative aspects of medical care, such as fairness of medical services, patient satisfaction, etc., in addition to patient survival rates.
In summary, the results of this study suggest that the most efficient utilization of the limited manpower of EM specialists requires that they care for patients with severe-to-moderate illness (levels 1 to 3). While this change would increase the average duration of ED stay, it could significantly lower in-hospital mortality risks. This study demonstrates the improved efficiency of utilizing EM residents rather than EM specialists to supervise patients with mild illness (levels 4 and 5) due to increased manpower, connectivity with other departments, and utilization of training physicians (interns).