In the field of emergency medicine our view of the circulatory system, for better or worse, has primarily focused on the function of the left ventricle. And yet the vast majority of patients in shock that we encounter in the emergency department have normal intrinsic ventricular function, rather suffer from an insufficiency in venous return.
In 1955 Dr. Arthur Guyton, the noted America physiologist, published a paper in which he described the factors that influence venous return physiology [1]. In this paper he highlighted three variables all of which independently affect venous return. These factors include: the right atrial pressure, the mean systemic pressure (Pms) and the vascular resistance [1]. The Guyton model of venous return is a complex and intricate system, and a detailed and expansive explanation is beyond the scope of this paper. Instead we will focus our attention on the Pms, its components, and its impact on venous return.
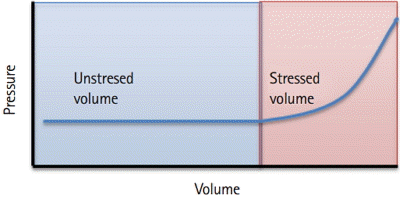
The Pms is an elusive concept that likely does not get the attention it deserves. This may be due to the difficulties encountered when attempting to define its importance or measure its existence. The Pms is the driving pressure competing against right atrial pressure to create a gradient that promotes forward flow. It is essentially the pressure measured in the vascular system if all blood flow were to cease [2]. The Pms is determined by the total volume of blood present in the venous system, and the intrinsic compliance of the vascular bed. In reality it takes a certain volume of fluid to fill the vascular bed to the point where its presence exerts force on the vessel walls. This is what is known as the unstressed volume. Any volume above this level is the stressed volume, which will exert an increasing degree of pressure on the venous vascular bed (Fig. 1). The greater the stressed volume, the greater Pms , and in turn, the greater the venous return [2].
Imagine a bathtub three quarters to capacity with the stopper located halfway up the side of the tub (rather than at the base). The stopper is unplugged and a drainpipe is inserted which leads to a bucket. The flow of water from the bathtub (vasculature) to Unstressed volume the bucket (the right atrium), is determined by the relative pressure between the tub (the Pms), the bucket (the right atrial pressure) as well as the length and diameter of the drainpipe (venous resistance) (Fig. 2). In this model, the tub will drain to the level of the drainpipe but no farther. The remainder of the water in the system is considered the unstressed volume. In order to get more water to flow from the tub to the bucket, either more water can be added to the system, increasing both the total volume and stressed volume, or one can compress the walls of the tub. This will decrease the systemŌĆÖs compliance, shifting a portion of the unstressed volume into stressed volume, which will allow more water to drain from the bed without adding additional volume to the system.
Let us examine this model in a clinical setting such as septic shock. The hypotension observed in sepsis is typically a distributive process. Essentially the vascular bed has vasodilated causing a relative hypovolemia. The total volume status is unchanged, but the vasodilation has caused an increase in the vascular compliance. This shifts a portion of the stressed volume to an unstressed state, leading to a decrease in the Pms, and in turn the venous return [3].
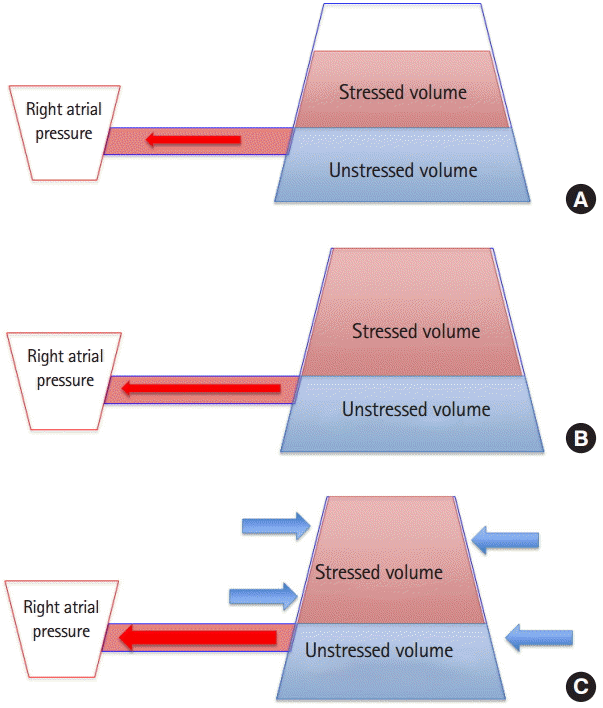
In the hopes of correcting the physiologic perturbations induced by the septic state, it is not uncommon to attempt to implement changes by manipulating the stressed volume. Typically this is done in two fashions. First, one can add to the total volume of the system (in the form of a fluid bolus), which will increase both the stressed volume and the total volume. Second, one can promote a reduction in the vessel wall compliance (with the addition of vasopressor agents), causing a change in the ratio of volume in the stressed and unstressed states. In this case the total volume would stay constant, while the unstressed volume decreases and the stressed volume increases.
Now instead let us examine the effects of hemorrhagic shock on the stressed and unstressed volume. In acute blood loss the total volume will be reduced, leading to a decrease in the stressed volume. In the initial phases of compensated shock the body attempts to adapt for this loss with a catecholamine-induced venoconstriction. This compensatory measure decreases the compliance of the venous system shifting blood from the unstressed to the stressed volume, increasing the Pms and temporarily maintaining the venous return. If bleeding is not controlled, blood loss will outpace these compensatory venoconstrictive efforts. At this point further attempts to augment preload through the shifting of unstressed to stressed volume will not improve venous return. Volume replacement is now required. The replacement of lost blood with blood products, is an attempt to restore both the total volume and stressed volume to a more physiologic state [3].
The physiology behind venous return is extremely complex and employs many independent variables all working in an asynchronous fashion. Despite the stressed and unstressed volume being only one of the many concepts that influence venous return, an intimate understanding of their influences is vital to managing hypotension in the emergency department. Traditionally emergency physicians have focused on volume replacement as the primary method of augmenting preload in patients presenting in shock, regardless of initial volume status. As a result, many patients who may not be truly hypovolemic, receive large volume fluid resuscitations. We are learning that this high volume strategy may cause complications downstream in the patientŌĆÖs inpatient hospital course. Early use of low dose vasopressors (norepinephrine at 5 mcg/min) will result in a venoconstrictive effect, decreasing venous compliance, and shifting fluids from the unstressed venous beds to the useable stressed volume. Unless there is evidence of significant hypovolemia, administration of fluids should generally be limited to 20 to 30 mL/kg before vasopressors are considered.