INTRODUCTION
Clinicians are often faced with the scenario of predicting outcome in patients resuscitated from cardiac arrest. A recent meta-analyses demonstrated cortical, short latency somatosensory evoked potentials from median nerves (mSSEPs) are an independent factor associated with outcomes [1]. Also, the bilateral absence of the N20 response from cortical mSSEPs performed within the first week of resuscitation following cardiac arrest is an accurate predictor of death or poor neurologic outcome with close to 100% specificity [2]. However, in the hypothermia era, their false positives may be as high as 3% questioning their validity. Previous case reports have challenged the prognostic value of mSSEPs in isolation [3].
Short latency auditory evoked potentials have been used to evaluate brainstem function. The neural generators of their components are dispersed along this structure, and are sequentially activated when the cochlear cranial nerve is stimulated with sound at the ears. These brainstem auditory evoked potentials (BAEPs) are more resistant than mSSEPs to sedatives and anesthetics [4]. However, BAEPs have not demonstrated the same prognostic value in intensive care units (ICUs) as mSSEPs, demonstrating a specificity of 60% and a sensitivity of 47% at predicting poor outcomes after hypoxic-ischemic events [5]. This may be due to the fact that the brainstem is less frequently affected than the cortex after cardiac arrest [6,7].
CASE REPORT
A 34-year-old male was brought to the emergency department with a gunshot wound to the chest. Despite receiving 3 units of whole blood and multiple liters of intravenous fluids during his transport, the patient became hemodynamically unstable. Laboratory tests upon admission revealed as follows: Hb 7.3 g/dL, Hct 23%, Na 149 mEq/L, K 3.1 mEq/L, Cl 114 mEq/L, blood urea nitrogen 34 mg/dL, Cr 1.2 mg/dL; arterial gases (Fi 100%): pH 6.57, PaCO2 28, PaO2 216, HCO3 5; toxicology screening: negative. Thus, from hypovolemic shock he subsequently experienced a cardiac arrest for 10 minutes before receiving a thoracotomy with direct heart compressions.
After return of spontaneous circulation, the patient was taken to the operating room for repair of his injuries and closure of his thoracotomy. Upon arrival to the ICU he was still intubated and on full mechanical ventilation, with no active bleeding. He was maintained under the effects of general anesthetics and neuromuscular junction blockers
A non-contrasted head computed tomography showed mild signs of bilateral supra-tentorial brain edema. Differential diagnoses included 1) early manifestation of hypoxic-ischemic encephalopathy during the cardiac arrest, advanced reanimation, or surgical times; 2) positive fluid balance during the initial hospital stay; or 3) closed head trauma. Treatment was initiated with elevation of the head and midline neck positioning. In addition, he received a mannitol bolus (1 g/kg). Due to concerns for potential coagulopathy from resuscitation, the patient was not treated with therapeutic hypothermia, and was maintained at 37°C. He was sedated with propofol and monitored with continuous electroencephalography for 24 hours.
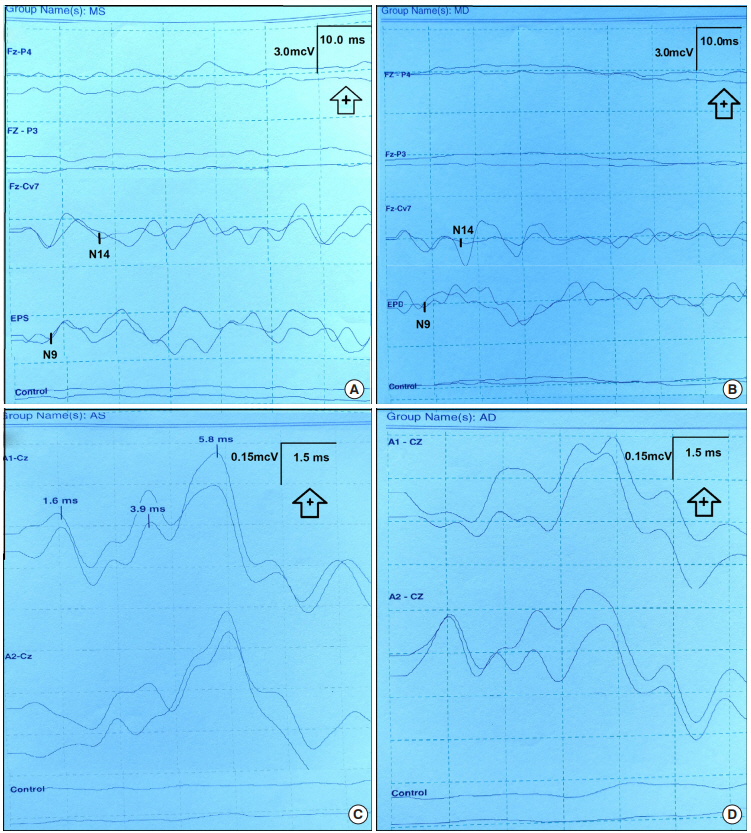
Over the next 2 days, the patient was weaned off vasopressor support and maintained a positive fluid balance. He continued to receive general supportive measures in the ICU without complications. Forty-eight hours after all sedatives and neuromuscular agents had been discontinued, he remained comatose. He was unresponsive to verbal or painful stimuli but demonstrated brainstem reflexes of direct and consensual photo-motors, corneal and gag. He had increased deep tendon reflexes (+++/++) in a generalized fashion and bilateral Babinski’s sign. On his 5th hospital day, mSSEPs and BAEPs for outcome prognostication were performed and are shown as Fig. 1.
After mSSEPs and BAEPs, arrangements were made with the patient’s family to discuss prognosis and goals of care. Due to logistical issues the meeting was delayed for 2 days. On the 7th hospital day, the patient began to follow commands reliably, first with his lower and then upper extremities. Repeat mSSEPs were obtained that day and are shown as Fig. 2A, B. Because the N20 response of the left hemisphere was still not normal, a final non-contrasted and a perfusion single photon emission computed tomographies were ordered and are shown as Fig. 2C, D.
The patient survived and was released on the 10th hospital day, with persistent weakness of his upper extremities. A diagnosis of post-shock man in the barrel syndrome with anterior watershed infarctions, and a left area of posterior brain hypo-perfusion was made. His cerebral performance category was 3 and the modified Rankin score 4 on discharge.
DISCUSSION
To provide a clearer picture of the role the neurophysiological tests played in the patient’s approach we consider a summary of the techniques used to collect them will help. The median nerves were independently stimulated at the ventral aspect of each wrist. Disposable surface electrodes were used with the cathode proximal to avoid anodal blockage. Constant, supra-threshold current square waves at 3.43 Hz frequency and 0.2 ms duration were delivered, once motor thresholds were obtained, confirmed by active hands flexion in a patient free of neuromuscular blockers. Two 512 trial epochs were collected through standard, disposable, scalp subdermal, mono-polar, steel needle electrodes. The N20/P30 cortical response was recorded from the ipsilateral and contralateral Parietal areas referenced to the midline Frontal site (P4/Fz and P3/Fz) from the modified 10-20 international system. The mastoid apophysis also referenced to the same site (M/Fz) was used instead of a spinous process of a cervical vertebra, to record the subcortical cervical (N13/P14) component of the upper extremity mSSEP, to avoid moving the patient from supine. Both Erb’s points referenced to each other (left Erb’s point/right Erb’s point) were used to collect the (N9/P10) peripheral responses. The bandpass filtering was 5 to 250 Hz with a 20 K gain for channels recording cortical responses, while 30 to 1,000 Hz with a gain of 50 K for sub-corticals. Five (5) KΩ was the maximum electrode impedance accepted. This montage resulted in a slight variation from that recommended by the International Federation of Clinical Neurophysiology for the clinical practice of upper extremity mSSEPs [8].
BAEPs were elicited by using sound clicks of 50 ms of mono-aural stimulation carried out through ear inserts at 95 dB-HL intensity and 17.6 Hz frequency. Alternating polarity (rarefaction/condensation) was used to reduce stimulus artifact and to cancel cochlear microphonics. The contralateral ear was stimulated at 65 dB-HL with white noise for masking purposes. Their recording was performed through standard, disposable, steel, mono-polar needle electrodes sub-dermally located at both ear lobes referenced to the vertex (A1/Cz and A2/Cz), from the modified 10-20 international system. Bandpass filtering used was 100 to 1,000 Hz with a 100 K gain. A thousand and twenty-four trials were averaged per epoch of two collected, and electrode impedances of 5 KΩ, the maximum accepted. This montage also resulted in a very similar one to that recommended by the International Federation of Clinical Neurophysiology for the clinical practice of BAEPs [9].
Anesthetic or sedative agents and low room temperature affect the quality of evoked potential recordings in ICUs. Although our patient was not treated with therapeutic hypothermia and was kept euthermic during his ICU stay, he received a propofol infusion. Propofol does not typically affect SSEPs’ amplitude when used at doses of less than 2.5 mg/kg. Likewise, it does not affect BAEPs’ amplitudes when used at concentrations between 10 and 50 μg/kg·min [4]. During critical illness states, propofol’s metabolism can extend to 40 minutes [10]. Thus, with normal initial BAEPs’ recordings (Fig. 1C, D), we expected no effect of propofol in our patient’s mSSEPs. Other circumstances in which initial bilateral absence of N20 responses from mSSEPs have been reported with survival or good neurological outcome are reversible hypoglycemic coma, viral encephalitis, carbamazepine intoxication, head trauma, and hemispheric infarction [11-13]. These were not present in our patient. The N20 waveform at the Left Parietal areas did not have a completely normal configuration in the second evaluation of this patient (Fig. 2B) suggesting a concurrent degree of cerebral hypoperfusion, also present at posterior watershed areas, consistent with a man in the barrel syndrome, in which patients are affected mostly in anterior watershed areas (Fig. 2C), as demonstrated by the predominant motor compromise of the upper extremities in this patient [14]. For all these reason, when discussing validity of neurophysiological studies, their reliability should always be mentioned.
The only existing studies have shown moderate inter-rater agreement, with average kappa levels of 0.30 to 0.72 [12,15], attributed mainly to noise in the signals. Noise was present in this case, predominantly in the neck and upper thoracic channels where electromyographic artifact is more frequent during examination in the supine patient not under neuromuscular blockade. Intra-rater reliability has better agreement with kappa levels of 0.84 [12]. Standardizing techniques, obtaining high signal-to-noise ratios, using appropriate filtering, and averaging, are still useful solutions to obtain valid results [15]. The limitations of only one evaluation with this electrophysiological test against several longitudinal observations, as well as, information obtained by different modalities of neurological evaluation, such as perfusion studies must be considered when establishing the prognosis for an individual patient. Thus, our case adds to the literature supporting multi-modal strategies for determining outcomes in post cardiac arrest patients.